From Lab to Life — Heart Implantation instead of Transplantation
Today, more than ever, artificial heart implantation is becoming an excellent, accessible solution for people suffering from extreme heart failure, the epidemic of the Western world. Patients no longer have to wait years for a donor heart. The third generation of artificial hearts is here, and accessibility is growing.
Amna Hijazi, a 69-year-old resident of Tamra, suffered from heart failure for nearly 18 years. During the course of her illness, she was treated in the Department of Cardiology at Rambam Health Care Campus. Over the years, her doctors knew how to adapt her treatment as needed. Like many patients with heart failure, Amna also suffered from a decline in heart function until her heart reached a state of severe dysfunction. The Rambam team, therefore, suggested that she undergo implantation of a device that would support the left ventricle of her heart.
“The first time I heard about the artificial heart, I was very suspicious. I understood my life was at risk, and that this was the most appropriate treatment for me,” explains Amna. “It took time to digest and process the information I had received from the medical staff. I consulted extensively with my family, and we received a detailed explanation regarding the nature of the process that I was supposed to go through and how the device would work. The clarity of the information, combined with the support of my family and a great deal of faith, convinced me to undergo the process. Following months of treatments to prepare my body, I had the surgery. Today the surgery is behind me and I feel excellent and full of gratitude for my family, who are always with me, as well as for the medical team, of course, which showed uncompromising professionalism and concern for me throughout this entire process.”
Western Epidemic
Over the years, heart failure has become one of the biggest epidemics plaguing the Western world. As opposed to other heart diseases, the rate of heart failure is increasing, and this is the “price” that the cardiology world is paying for successes in other areas, which lead to better survival rates following heart attacks, and for other heart disease patients. Heart failure is the main reason adults over 65 are hospitalized, and the disease frequency only increases with age.
It is estimated that approximately 2% of Israel’s elderly population suffers from heart failure – in other words, at least 100,000 people. The proportion of them with significant functional decline and high mortality risk is 5% – around 5,000 patients each year. In the United States, these rates increase to 2.8% of the elderly population – close to five million people with heart failure, 10% of which already require advanced treatments.
Treatment, Not Healing
In most cases, patients receive treatments that maintain stability and normal heart functionality for years. However, they are not a permanent solution. Eventually, they will reach the stage where the initial solution no longer works and a new treatment must be found. “Even though there are many medications and solutions for heart failure patients that successfully keep the patient alive for years, there can still be a deterioration in their condition to the point where medications no longer help and the patient is at high risk. It’s important to identify this situation in time and offer treatments that include heart transplantation or a device that assists the left ventricle,” explains cardiologist Dr. Oren Caspi, who heads the advanced heart failure program at Rambam. “In the current case, the patient was treated by our heart failure team for many months and underwent a thorough, lengthy preparation and treatment process prior to the transplantation. It’s very important to refer every patient to a treatment center specializing in heart failure so they can receive the most suitable treatment at the right time.”
Only 20-25 heart transplantations are performed in Israel each year, but the waiting list has approximately 100 patients on it at any given time (according to a report from the Ministry of Health). Each year, many patients find themselves in the nerve-wracking wait for a heart transplant, knowing that the chance of receiving one is low. In addition to donor heart transplantation, which has existed for years, today there is the option for implantation of a left ventricular assist device, sometimes referred to as an “artificial heart.” This treatment is suitable for patients suffering from heart failure with a serious decline in left ventricular function, where the right ventricular function hasn’t deteriorated to the same extent (95% of heart failure patients). At first, this treatment was clumsy, but with today’s technological advances, the treatment is much more effective, safe, and accessible. If until a decade ago, an artificial heart for most patients was a temporary solution until a donor heart could be found, today, the development of third-generation “artificial hearts” and implantation devices means there is an excellent solution for many patients, including for those who require an actual heart but whose medical condition makes such a transplant impossible.
“The third generation of artificial hearts is a special pump that supports the activities of the heart’s left ventricle. It’s called an LVAD (Left Ventricular Assist Device),” explains Dr. Caspi. “The pump is a centrifuge implanted in the heart that does approximately 5,000-6,000 revolutions per minute. It pumps blood from the left ventricle into the aorta and maintains continuous blood flow to the entire body, assisting and replacing left ventricular functionality. A thin cable runs from the pump to the patient’s abdominal wall through the skin and connects batteries that charge the pump. It’s important to emphasize that this is treatment is suitable for patients whose right ventricles are still functioning well. As such, it’s important that they come for treatment before that function is also affected.”
The Key to Success, Preparation
“LVAD transplant surgery requires a very extensive preparatory process,” notes Dr. Tzvi Adler, a senior physician in the Department of Cardiac Surgery at Rambam and Amna’s surgeon. “In cases of this nature, you must prepare the patient, providing appropriate treatment that will prepare their body and enable them to survive the surgery and to function successfully with the pump. The process we went through with Amna in preparation for the surgery took many months, during which she received personalized treatment that stabilized and prepared her to physically handle this type of surgery. For the patient to receive the proper, precise treatment, it is important for them to come to a leading hospital cardiology center. The complexity of the long process requires professionalism and expertise. Our treatment teams, like those in other centers, underwent extensive training in Israel and abroad, and today they know how to prepare the patient.”
Professor Gil Bolotin, Director of the Department of Cardiac Surgery at Rambam, explains that studies today show that the survival rates following artificial heart implantation are identical to those for donor heart transplantation. “This is some of the data presented at the conference ‘Present and Future in Cardiac Surgery’, which was held at Rambam this month.” Research published recently in the world-renowned New England Journal of Medicine shows that in a two-year follow-up, survival rates of patients who underwent artificial heart implantation surgeries were the same as those for donor heart transplantation. “The research results are very encouraging, as artificial heart implantation surgery can serve as a replacement for patients who need a donor heart as well as a solution for patients who are ineligible for heart transplants,” adds Dr. Adler.
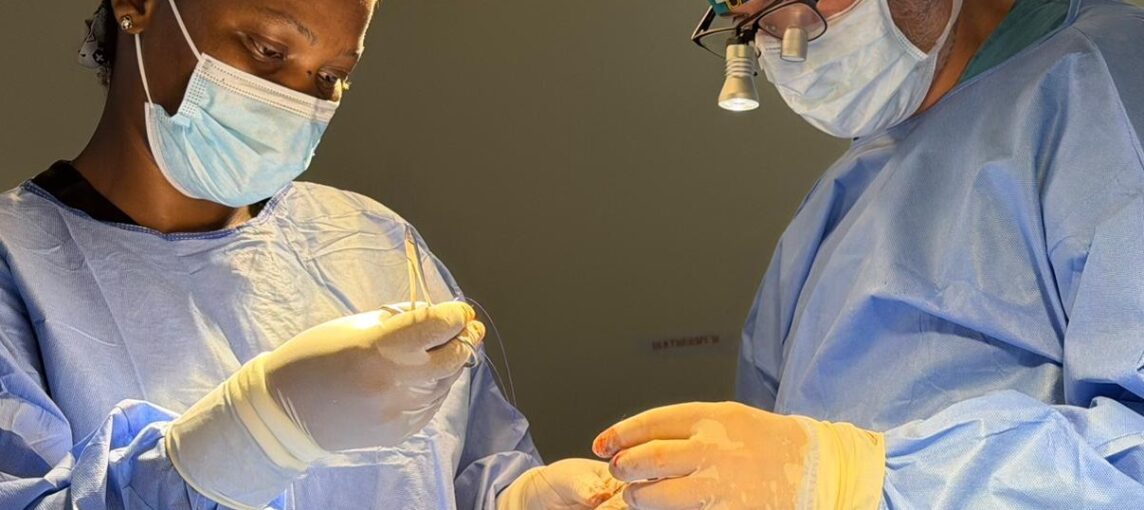
In the photo: Amna Hijazi with Dr. Oren Caspi (on the right) and Dr. Zvi Adler.
Photo credit: Nathaniel Ayzik